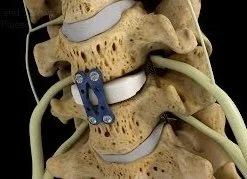
Anterior Cervical Disectomy and Fusion (ACDF)
-
Walking: Begin walking as soon as possible after surgery. Short, frequent walks are encouraged and help improve circulation, reduce stiffness, and lower the risk of blood clots.
Neck Motion / Restrictions: Avoid excessive neck bending, twisting, or jerking movements. If you were provided a cervical collar, wear it as instructed. Please see the additional sheet for information. Do not remove it unless cleared by your surgeon.
Lifting: Do not lift anything heavier than 10 pounds for the first 4–6 weeks. Avoid pushing, pulling, or overhead lifting.
Driving: Do not drive while taking narcotic pain medications or while wearing a cervical collar. Driving may typically resume 2–4 weeks after surgery once you have adequate neck mobility and are cleared by your surgeon.
Work & Daily Activities: Light-duty or desk work may be resumed in 2 weeks, depending on symptoms. Jobs requiring physical labor, heavy lifting, or prolonged neck strain should be avoided for at least 8-12 weeks or until cleared.
-
Keep the incision clean and dry at all times.
You may shower 24 hours after surgery if there is no drainage, but do not scrub the incision or allow direct water pressure.
Do not submerge the incision in a bathtub, pool, or hot tub for 4 weeks.
The surgical glue will flake off by itself; do not pull them off.
Avoid applying lotions, creams, or ointments to the incision unless directed.
-
Pain Medications:
Take prescribed pain medications exactly as directed. As pain improves, transition to over-the-counter medications such as acetaminophen if appropriate.Anti-inflammatory Medications:
Avoid NSAIDs (ibuprofen, naproxen, etc.) unless specifically approved, as these may interfere with bone fusion.Ice Application:
Ice packs may be applied to the neck or shoulder area for 15–20 minutes at a time to reduce pain and muscle tightness. Avoid heat unless instructed. AVOID HEAD PACKS.Muscle Spasms:
Muscle tightness in the neck and shoulders is common. Prescribed muscle relaxants, gentle walking, and posture awareness can help.Medication Provided:
o Oxycodone- Narcotic for pain for as needed use
o Cyclobenzaprine- Muscle Relaxant for as needed use
o Ondansetron- Anti-nausea medication to be used as needed
-
Mild difficulty swallowing, hoarseness, or a sore throat is common after ACDF and usually improves over days to week.
Eat soft foods initially and take small bites.
Stay well hydrated.
Notify your surgeon if swallowing difficulty worsens, breathing becomes difficult, or symptoms do not improve.
-
Constipation is common due to anesthesia and pain medications.
Drink plenty of fluids.
Eat fiber-rich foods (fruits, vegetables, whole grains).
Consider stool softeners (e.g., docusate) or mild laxatives if needed.
-
Call your doctor immediately if you experience:
Fever above 101°F (38.3°C).
Progressively increasing pain that is not relieved with medication.
New or worsening numbness, tingling, or weakness in your legs.
Loss of bladder or bowel control.
Redness, swelling, or drainage at the incision site.
Trouble breathing or swallowing
-
Your first post-operative visit is typically scheduled 2–3 weeks after surgery.
X-Ray will be performed at 3 months and a CT of the cervical spine at 6 months
If prescribed, set up Physical Therapy for ~2 weeks after Surgery
Avoid high-impact activities, running, or contact sports until fully cleared—often 3 months or longer, depending on fusion progress.
-
If you have any concerns or questions, please contact our office.
Emergency Contact Information:
Washington Brain and Spine Clinic- 301-718-9611
Email: LDaggubati@brainsurgery.com
Timeline for Optimized Recovery
-
Neck Protection & Alignment
Cervical collar (if prescribed):
Wear as directed (often continuously for the first 2–6 weeks except for hygiene).
Maintain neutral alignment—avoid excessive flexion/extension.
Sleep:
Use a firm pillow or cervical roll.
Supine or side-lying positions only; avoid stomach sleeping.
Wound & Swallowing Care
Keep incision clean and dry.
Mild dysphagia is common (especially C5–6, C6–7 levels).
Small bites, soft foods, adequate hydration.
Call if progressive dysphagia, aspiration, or inability to tolerate diet.
Pain Control (Multimodal)
Scheduled acetaminophen (baseline analgesia).
Short-course opioids only as needed.
Muscle relaxants for spasms.
Avoid NSAIDs (generally 6–12 weeks) due to fusion inhibition risk.
Ice to the posterior neck/shoulders (not directly over incision).
-
Activity
Walking daily is the single most important activity:
Start short and frequent (5–10 min, 3–4×/day).
Gradually increase duration.
Avoid:
Lifting >10 lbs.
Overhead reaching.
Sudden neck rotation or extension.
Posture & Ergonomics
Maintain neutral cervical posture:
Screen at eye level: Avoid prolonged phone or laptop flexion (“text neck”).
Lumbar support when seated.
-
Nutrition
Protein intake: ~1.2–1.5 g/kg/day.
Calcium: ~1,000–1,200 mg/day (diet + supplement).
Vitamin D: Target serum 25-OH >30 ng/mL.
Ensure adequate calories—avoid aggressive dieting early.
Smoking & Nicotine
Absolute avoidance of:
Cigarettes
Vaping
Nicotine patches/gum
Nicotine significantly increases pseudoarthrosis risk.
Medications to Avoid
NSAIDs (ibuprofen, naproxen, celecoxib) unless surgeon-approved.
Chronic steroids if avoidable.
-
Weeks 2–6 (Surgeon-Directed)
Gentle range of motion (if cleared).
Scapular stabilization.
Isometric cervical strengthening.
Postural re-education.
Weeks 8–12
Progressive resistance.
Deep neck flexor training.
Core strengthening.
Avoid axial loading until fusion evidence.
-
Activity
Desk work 2–4 weeks
Light duty 4–6 weeks
Manual labor 8–12+ weeks
Driving Off narcotics + good ROM (~1 month)
Sports/gym After fusion evidence
-
Bone growth stimulators (multi-level fusion, smokers, osteopenia).
DEXA screening in older or high-risk patients
Sleep optimization (OSA management if applicable).
